Every 12 seconds, a woman is abused by her intimate partner here in the U.S. Among all women, an eye-popping 53 percent report that they have experienced abusive behavior from a partner, with one in four women experiencing severe physical violence in an intimate relationship.
Years after the bruises from domestic violence fade, the resulting physical effects can stick around in the form of serious health issues, everything from debilitating migraines, hypertension and chronic back pain, to severe arthritis, diabetes and even gastrointestinal diseases like irritable bowel syndrome.
Women who had left their abusers years, even decades, ago – thinking that chapter of their lives was closed and behind them – now face far higher than normal rates of chronic health problems. Some studies have shown that abused women have 2.7 chronic conditions per person versus 1.7 chronic conditions for women who have never experienced abuse. The higher number of chronic conditions for abused women result in medical expenditures of nearly 20 percent above what other women spend.
So why are these women having to deal with chronic health problems when they have been away from the abuse cycle for so long? New research may hold the answer:
Domestic Violence and Chronic Illness
Michele Black, an epidemiologist for the Centers for Disease Control and Prevention and lead author for the groundbreaking 2011 study on domestic violence related illness, recently stated for More magazine that “A woman in a violent relationship is often on high alert. She may be frightened about being killed or worried about her kids. If she tries to get away, she may be stalked. All that stress is really toxic. There’s no organ that’s immune. Your whole body is at risk.”
Here is a quick comparison chart from that ground-breaking study to show you the difference between chronic illnesses reported by abuse survivors and those who never experienced abuse:
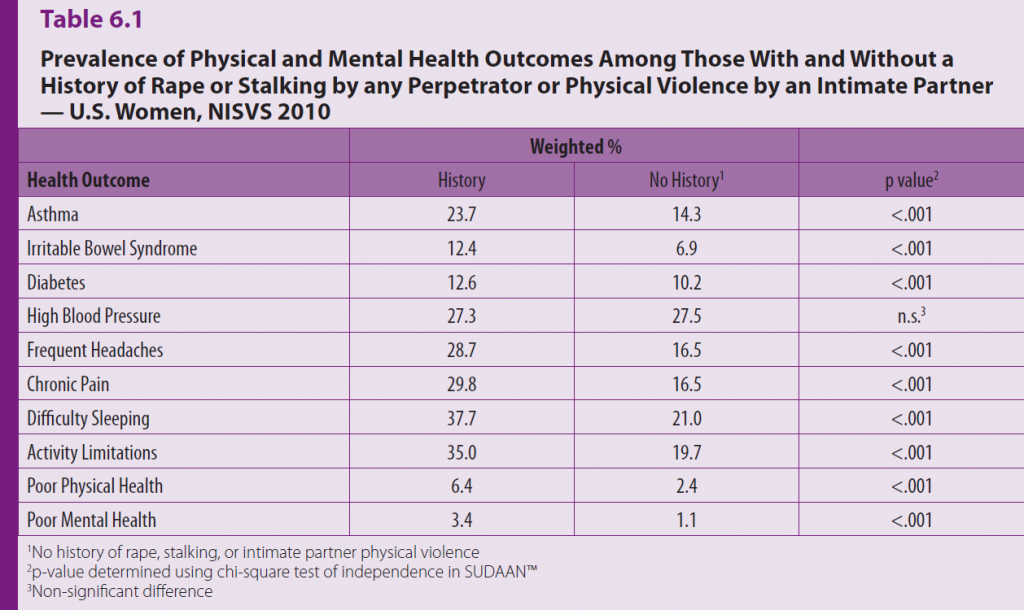
When someone is injured, the body’s “super-system” (immune, nervous, and endocrine systems) works to meet the challenge of wounding, defend against the threat to the body, and resolve the wound by healing. If the injured person is exposed to repeated attacks or experiences a high-trauma event, the “super-system” can overload and stay in a constant state of overload, which keeps it from healing the injury, leading to chronic health issues.
Such damage can impair brain function, the endocrine system, the immune response, and even DNA. A recent study at the School of Nursing at the University of California (San Francisco) found that women who have endured long periods of abuse, especially if they had young children at the time, tend to have shorter telomeres, when compared to women who have not experienced abuse. Telomeres are the strands of DNA that protectively cap the ends of chromosomes. In response to severe, chronic stress, telomeres tend to shorten, which can lead to premature cell death. Even years later, after having long left their abusers, these victimized women often have the physiological profile of women 10 years older.
Researchers have also learned that abuse-related injury, the severity of post-traumatic stress disorder (PTSD), and the severity of depression all have an impact on chronic pain in women who suffered not only intimate partner violence but also child abuse as a young child. A woman who experienced both child abuse and IPV is also at more than double the risk of experiencing PTSD than a woman who only experienced child abuse or adult victimization. The intensity of the pain, the emotional distress, and the amount of physical disability are greater in women with chronic pain who also have PTSD.
Movement Within the Medical Community
For many years, the medical community (in large part) turned a blind eye towards the cause of injuries in abused women. Even worse, they would attend to the injury without questioning the victim about prior abuse-related injuries, leaving fractured bones and traumatized areas of the body from past injuries undocumented and unattended. These old injuries would develop into chronic pain centers later in the victim’s life.
Now all that is changing. Emergency rooms and doctors around the country have intimate-partner violence on their radar. In January 2014, the U.S. Preventive Services Task Force (an independent panel of experts) called for doctors to screen all women of child-bearing age for IPV. Doctors, having been made aware of the immunology research behind post-abuse health issues, realize the importance of screening and developing effective interventions to help minimize the future impact on the victim’s health.
Promoting Awareness, Understanding and Compassion
Organizations like nomore.org and the National Coalition Against Domestic Violence (NCADV) work hard to spread the message about domestic violence and reporting. With the help of these organizations and others like them, the public awareness of domestic violence and intimate-partner violence is growing, helping Americans nationwide to have greater understanding and compassion towards DV abuse victims and chronic illnesses.
If you are a victim and survivor of domestic violence and are experiencing chronic illness, know that your condition is most likely a result of past abuse. Years of staying on high alert and enduring abuse have taken a toll on your body.
If you know someone who has chronic illnesses, be more kind, understanding, and compassionate. That person just might be suffering from current or past abuse.
(Photo Credit: doctor_patient via Compfight cc)